Elise D. Machrone*
University of Washington, Seattle, WA
______________________________________________________________________________
ABSTRACT
Do you love having a cafè-au-lait to start your day? While so many of us indulge in the creamy mixture of milk and espresso, the general public is unaware of the de-caffeinated, dermatological connotations of this word. This article will share my personal experience with cafè-au-lait spots and reveal the complexities of this skin condition that can indicate a much more serious disease called neurofibromatosis. So, let’s remove the caffeine —for now— and talk about skin.
______________________________________________________________________________
When I was ten years old my observant pediatrician noticed freckles in one of my armpits suddenly making an appearance to complement my previously existing patches of flat, pigmented macules in other areas of my body. With visible concern, she urged my parents to take me to a dermatologist. A University of California Los Angeles (UCLA) specialist quickly defined a number of patches as cafè-au-lait spots after a thorough full-body examination. It is appropriate to note that these macules alone are harmless and simply appear as light brown areas on the skin that are visibly darker than surrounding skin. Their shape can either be several small freckles, larger patches, which sometimes cover areas of the body. If you have just one to three café au lait spots, doctors forgo further assessment; however, spots requiring further testing form in around 10-20% of individuals [5]. Patients falling within this category are either born with them, or develop them during childhood. I had 5 cafè-au-lait spots of concern in addition to the newly forming freckles under my arm.
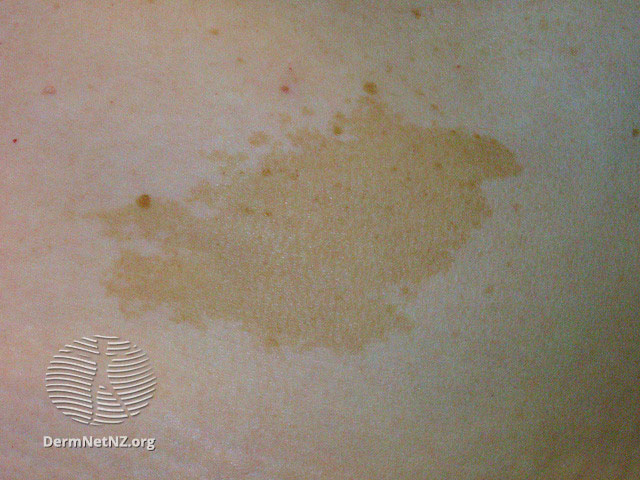
Prior to learning about diseases attached to cafè-au-lait spots, many think they are simply unique birthmarks and pretty “cool” to look at. However, when combined with other observations, doctors develop concern since these spots can have strong ties to neurofibromatosis—specifically in my case “segmental” neurofibromatosis which became increasingly important to monitor. Next, I was referred to a top UCLA geneticist for an in-depth examination; but first let’s review a bit more about this disease that can be discovered from clues on the skin.
While neurofibromatosis can be passed through family genetics, segmental neurofibromatosis (type V neurofibromatosis) is a disease with no direct family history and no systematic growth that is distinguished solely through cafè-au-lait macules and neurofibromas. It can occur from a genetic alteration in utero before birth. The disease was scientifically defined by Riccardi in 1982 after several variations of neurofibromatosis had been reported; neurofibromatosis was originally the broad term, however, the 8 variations of this disease led Drs. Miller and Sparks to coin the term “segmental neurofibromatosis”[3]. Segmental neurofibromatosis means that the signs and symptoms are limited to a certain area of the body and only some cells are affected.
Let’s examine a 2014 case study by Drs. Sobjanek, et. al., from the Department of Dermatology at the Medical University of Gdansk, Poland. A 63-year-old Caucasian woman showed doctors her 20-year-old nodule growth contained in the right lumbar. When looking at the figures uploaded by Sobjanek, I see that the patient’s nodules are abundant, both soft and firm, with a flesh color and dome shape. They vary in size and are not spread throughout the patients lumbar, but stop right at the patients vertebral column. The patient had excised tumors which displayed neurofibromas after histopathologic review. Although segmental neurofibromatosis is often accompanied by neurological and ophthalmologic symptoms, they were not present in this case [1]. This particular study indicates that there are many variants of segmental neurofibromatosis and dermatologists cannot expect all patients to show symptoms in the same manner.
Several alarming symptoms of segmental neurofibromatosis, which extend beyond the previous patient example, exist and they can take many forms. One malignancy associated with segmental neurofibromatosis is a peripheral nerve sheath tumor, which is a cancer of the cells which form a sheath that provides crucial protection to peripheral nerves. The nerves which extend outside the central nervous system of the brain and spine define these peripheral nerves. Malignant melanoma, another potential risk, is the most serious type of skin cancer where our pigment producing cells become cancerous. As a result, new and changing moles become visible. Further, Hodgkin lymphoma limits the body’s ability to fight infection causing fatigue, swelling of lymph nodes, fever. Other malignancies include colon cancer, gastric cancer, and lung cancer.
Beyond the physically damaging consequences, neurofibromatosis can cause cognitive deficits during childhood. With this comes challenges in academic achievements. Shelly L. Hyman, a neurologist, provides an insightful analysis. She studied 81 children, 43 males and 38 females, who have NF1 and found that 52% of the children had academic achievement challenges, with only 20% diagnosed with a specific learning disability. This meant that 32% had general learning problems: not strongly correlated to neurofibromatosis. Patients diagnosed with neurofibromatosis are thus shown to have varying symptoms [3].
How does gender affect neurological reactions to this disease? While not conclusive, it was interesting that after data was run, specific learning disabilities were solely present in male participants from this cohort. Diagnosis of a specific learning disability was made through discrepancies in the VerbalIQ<PerformanceIQ test [5].
Fortunately, in my case I had impressed my teachers with strong academic marks from a young age and show no sign to date of the harmful mental or physical signs of the disease. There were no nodules on the surface of my skin. My family and I are greatly relieved. However, nodules may develop just below the skin, in deeper skin tissues, or in internal organs. Moreover, there is additional risk as a patient enters puberty that further symptoms may appear.
Since my parents are vigilant, they proceeded with the recommended tests, including a full body MRI to help doctors develop an accurate diagnosis. My innocent childhood self remained blissfully unaware of any potential medical challenges. In contrast, my parents were gripped with fear as they watched their little girl play happily with her friends week after week. We continued to delve into subsequent eye examinations, an MRI, and blood tests throughout the coming months to alleviate their concerns.
The first analysis was a specific ophthalmological evaluation for both myself and my mother which uncovered another clue in my medical puzzle—lisch nodules, which are ocular phenomena indicating NF1. Since my maternal family appeared to have a few potential indicators, my mother was also given an exam. One lisch nodule was discovered in my mother’s left eye and 2 pigmented spots were visible in my left eye which have since turned into a shaded area that continues to be monitored each year.
Next, I found myself lying in a giant chamber listening to music for one hour while my mom patted my head and an MRI detailed images of my entire body; doctors targeted my abdomen and chest looking for plexiform neurofibromas as well as any additional lesions associated with NF1. Once completed, my doctors were relieved to share that I had no signs of internal neurofibroma. Fortunately, I also tested negative for constitutional, eyes, ENT, respiratory, cardiovascular, genitourinary, musculoskeletal, neurologic, psychiatric, endocrine, hermatologic, allergic, and immunologic system issues.
Further, blood tests are of utmost importance to analyze the presence of harmful body conditions. A highly targeted genetic blood test indicated a benign anomaly for my mother but nothing unusual was found for me. At that point, concluding all reasonable modern tests and with no other indicators, the segmental neurofibromatosis diagnosis was considered at-most borderline for me. A huge weight was lifted.
Since that young age I have continuously had full body skin exams every six months to examine potential growth of existing cafè-au-lait macules and formation of new spots. In addition, my eyes are assessed every year to look for lisch nodule development. With the capabilities of technology today doctors have turned to the use of iPads and computers to record valuable information during examinations. Each dermatology appointment typically involves a headshot of my face and subsequent pictures of my spots. This allows my doctor to easily access a record of my skin macules and effectively compare them with new images when I return for each visit.
The expansion of technology in medicine has been astounding and has made an impact in our recent medical advancements. This technology did in fact find that one of my spots had changed color and shape. As a precaution, my dermatologist performed an outpatient pendulum biopsy—a punch tool scoops skin like a pendulum—and sent the lesion to a lab for examination. Some biopsies require stitches, but I was instructed to keep my open wound under a large bandaid and use a Q-tip with alcohol to ensure proper healing, always keeping the area out of the sun as new skin is susceptible to burning and could cause hyperpigmentation [4].
Once in the lab, the skin biopsy sample is carefully examined by a dermatopathologist under a microscope. The delicate piece of skin is “carefully embedded into paraffin wax”(Dr. Bologna of Yale Medicine’s Dermatopathology lab). This develops a block, which can be carefully cut to be placed on glass slides. The pathology lab uses an array of stains, with Yale Medicine’s Dermatopathology lab having over 250 stains for skin alone. Some of the most challenging medical cases are discussed in a daily consensus council, where dermatopathologists share their opinions and analyze related literature, in order to form an accurate diagnosis. Dermatopathologists look for abnormally dark and large nuclei to determine cancerous cells, those with darker nuclei than non-cancerous cells. What makes the nuclei darker and larger? Cancerous cells have more DNA than non-cancerous cells [6].With the separation between the dermatopathologist and patient, often the dermatopathologist will reach out to the dermatologist in order to learn more about the patient’s medications and medical disease history [6]. If a melanoma is ultimately diagnosed, “the area must be re-excised”.
I am thankful that my cafè-au-lait macules have remained benign through the years and I am optimistic that research continues to offer dermatologists a better understanding of their history and potential impact. Although there is not one simple list to check off for neurofibromatosis due to the variability of the disease, more research can improve the accuracy and credibility of one’s path to a healthy body even when some risk factors are discovered.
We all must remember that our skin is the biggest organ in our body. We must take care of it. We must learn about it. And, as I have shared today, it is of the utmost importance to understand all connotations of the famous, cafè-au-lait.
- Author Bio: Elise Machrone grew up in Los Angeles and is a passionate pre-med at the University of Washington. She has spent her summer volunteering at Cedars-Sinai Medical Center, teaching math to students at Mathnasium, and studying economics. In her free time, she loves photography, writes articles and poems, travels, goes on walks with her French bulldog, and cooks for her family. She is excited about all that awaits her in college and beyond.
______________________________________________________________________________
REFERENCE
- (PDF) Segmental Neurofibromatosis – Researchgate. https://www.researchgate.net/publication/271335023_Segmental_neurofibromatosis.
- “Café Au Lait Spot.” Café Au Lait Spot – an Overview | ScienceDirect Topics, https://www.sciencedirect.com/topics/medicine-and-dentistry/cafe-au-lait-spot.
- Gabhane, Sushma Kashinath, et al. “Segmental Neurofibromatosis: A Report of 3 Cases.” Indian Journal of Dermatology, Medknow Publications, 2010, https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2856359/.
- “How Is Cancer Diagnosed?” American Cancer Society, https://www.cancer.org/treatment/understanding-your-diagnosis/tests/testing-biopsy-and-cytology-specimens-for-cancer/how-is-cancer-diagnosed.html.
- KN;, Hyman SL;Arthur Shores E;North. “Learning Disabilities in Children with Neurofibromatosis Type 1: Subtypes, Cognitive Profile, and Attention-Deficit-Hyperactivity Disorder.” Developmental Medicine and Child Neurology, U.S. National Library of Medicine, https://pubmed.ncbi.nlm.nih.gov/17109785/.
- “Skin Biopsies: What You Should Expect.” Yale Medicine, Yale Medicine, 27 Nov. 2017, https://www.yalemedicine.org/news/skin-biopsy.

